This Date in UCSF History: Practicing Medicine Under Hardship
Originally written by medical student Amy Ewing and published in Synapse on November 6, 1997.
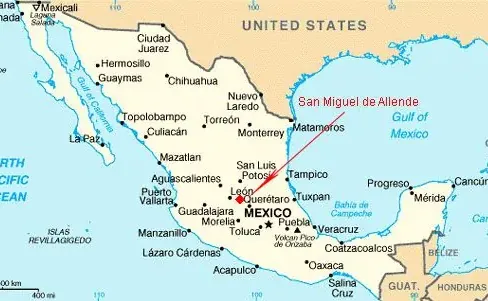
Last year I arranged to spend the month of July working at two small hospitals in San Miguel, a town of 50,000 people in the highlands of central Mexico. I went hoping to learn how Mexican-born patients, who would make up much of my practice here, are cared for at home for common problems like diabetes, hypertension and stroke.
I thought I’d improve my medical Spanish, see a few local health problems, and begin to understand my patients’ experience with the healthcare system of their homeland. The doctors I met helped me reach these goals.
More importantly, they taught me about Mexico’s precarious public health care systems. And they eloquently communicated the heartbreak of trying to provide care, maintain skills and make a living as a public servant in a bankrupt economy. Their situation is now getting even harder, as I found when I returned there in July 1997.
Haves and have-nots
My introduction to health care in the state of Guanajuato came about through friends who knew a cardiologist there. This doctor welcomed me to a brand-new 15-bed hospital built to serve wealthy insured patients and pointed out its advantages over the nearby hospital civil, a publicly funded hospital serving state employees and the poor. The private hospital was impressive and new — but it was almost empty, and its doctors were protective of their patients.
The hospital civil was run-down and overcrowded. The contrast was familiar: a local re-enactment of the familiar contrast between UCSF and the General. When I realized that Guanajuato’s “UCSF” was only getting about three ER visitors a night (because almost no one in post-recession Mexico can afford insurance) I asked to watch some doctors in the ER at the hospital civil. I was very lucky that its director agreed, despite my lack of formal documents, to let me observe informally in their ER and OR. I happily stayed for the next month.
Common diseases are major killers
The hospital receives referrals from a network of rural clinics which covers the northeast corner of the state of Guanajuato, an area about the size of the Bay Area and one of the most economically depressed in the country. It is very arid.
Many water sources in the area are contaminated with amoebas, Giardia, or Shigella. Cholera has recently become endemic there. Late in the season, water supplies dry up and the bacteria become concentrated. Both children and adults become ill. Guanajuato’s infant mortality rales from respiratory disease and diarrhea are among the highest in the country.
I saw women with poisoned spider bites, children with elbows broken from falling off the family’s donkey, and men with lung abscesses full of amoebas that had migrated up through their diaphragms. And I saw the struggles and achievements of a system persisting despite profound financial trouble.
I had three excellent mentors: an internist, a pediatrician, and a general surgeon. On my first day, they invited me to join a seminar they were giving to a group of 11 young Mexican doctors, each assigned to a rural clinic in the region.
The seminar was designed by the state of Guanajuato to help rural clinic doctors stay up to date on disease treatments, educate rural mothers in prevention, and get the worst cases to a hospital in time to save their lives. It was very practical. In a small, hot room, we reviewed drugs and dosages, treatments for rehydration, and how to make your own infant rehydration formula. We discussed when to call an ambulance and how to keep a child from dying en route.
In Mexico, as in most of the world, medicine is a four-year undergraduate course. My young doctor classmates were 23-year-old medical school graduates, starting the mandatory year of national public service. They are known as medicos pasantes.
Each single-handedly staffed a one-room clinic in a village four to eight hours away, down dirt roads, served by no independent transportation. Their resources were primarily the few books, microscopes and experience they had brought with them.
Their main job was to take care of small injuries and infections, stock and prescribe a few antibiotics, and triage and stabilize truly ill patients for the long, bumpy ambulance ride to a primary care clinic in San Luis, about two hours from here, or all the way to the secondary care hospital in San Miguel.
They were all glad to have a few days to be in town, go dancing, and get reacquainted. Nearly all of them had all recently graduated from urban medical schools and been randomly assigned to this area. None of them could afford cars.
Aurelia, from Mexico City, told me about living in a cluster of adobe homes without a communal building or store, rotating meals in her neighbors’ homes, and sleeping on a bed in the middle of her examining room.
Evangelio and Monica, who were sweethearts, were fortunate enough to be a 45-minute walk from each other. The other young doctors in the group would probably not see each other again for several weeks after our course ended. The area was going through a major drought, so diarrhea cases were going up, and their funds had been hit hard by the devaluation of the peso.
Their tiny stipends don’t permit them to leave very often during the 36 hours they had off each week.
The medicos pasantes and other doctors I spoke with gave me a basic explanation of Mexican medical education. First, medical school education is undergraduate, as it is in Europe. Admission to a university is dependent on national exam scores. But the choice of medicine as a career seems to be open to any university student. This makes sense because Mexico needs to create a large pool of primary care doctors. After graduation, there is the service year.
Then, all of my friends would lake another set of exams to determine whether they could specialize or not. If they did not pass, they would remain GPs. They all said they wanted the chance to specialize.
Mexican doctors’ salaries are about $6,000 to $8,000 a year — very low, even relative to the Mexican cost of living. Every doctor I spoke to had to supplement his or her salaried work by moonlighting in a private office, or by investing in labs or radiology equipment. Without a specialty, it is very difficult to supplement that income in any way. A specialist’s lifestyle can be very different.
In large city hospitals, which serve the 20% of Mexicans who can afford private health insurance, equipment and techniques match those we UCSF students use daily. At these hospitals, conditions may even be better than at UCSF.
A recent National Public Radio story interviewed patients in Mexico City who custom-order restaurant meals in rooms outfitted with hot tubs. The operating rooms and ICUs are fully equipped.
In contrast, at the hospital civil, the orthopedist brought in all his own instruments for each case. At the other hospital, the sole pulmonary physician had contributed the one intensive care monitor and took pieces of it home with him at night so that they would not be stolen.
I could see that it would be difficult, as a rural generalist, to stay current with medical practices. Medical journals are prohibitively expensive. In a town where the weekly salary for a four-day-a-week housekeeper was $22 U.S., food prices were equivalent to prices here.
In stores, hard-cover novels still cost $12-$20 U.S. Paying for medical journals for a private practice must be nearly impossible.
The class I attended was probably a good example of courses open to generalists. It was taught from overhead projectors. While there was a syllabus, the hospital could not afford to make photocopies of it. The students didn’t expect them, either. They simply took notes and then memorized them completely, including all of the drug dosages.
The pasante year makes it hard for students to maintain the skills they pick up in medical school. I could tell, because I had the opportunity to observe a group of residents after the pasante class left. An internist asked the residents to evaluate a young patient with a possible head injury and walked away. Nervously, they consulted with each other about how to test cranial nerves, and just how to evaluate pupillary changes. After their year of isolation, they were as lost as I was.
Hospitals in economic crisis
After two days of lectures, the pasante class was invited to round on patients with the instructors. I went with them and became more familiar with the hospital where I would spent most of my time in the next few weeks. The hospital building, which was one-story and contemporary, was laid out like an American junior high school. It had about 20 beds, a maternity ward, and a level I nursery.
About eight physicians were in charge during the day, with four or five others taking over from them at night. It was also a teaching hospital: shortly before I left, three residents came to join the team.
Mexico has undergone three years of one of its most severe economic crises. I had read about hospitals in the north where patient care has suffered recently, both due to lack of funds and due to more insidious problems, like underlying malnutrition. I was not sure what I would see in San Miguel, because the town is outwardly prosperous. But there is tremendous unemployment, and deep cuts in Mexico’s cash reserves have left the hospitals strapped for cash to buy anything made overseas.
The hospital civil was small, and quiet, and clean. It accommodates a lot of very impoverished patients and provides many services for free or next-to-nothing, since none of its patients have any insurance. Packets of infant rehydration formula were set out on the counters. Yet everything was designed for economical use or re-use. I never saw a pair of disposable gloves; they were all sterilizable.
When I was invited to scrub in for surgery, it caused a slight consternation when I admitted I hadn’t brought my own scrubs with me. It turned out that each physician is responsible for supplying his or her own scrubs. The hospital takes responsibility for sterilizing them. None of the physicians brought his or her own stethoscope; several were shared between the emergency room and the outpatient clinic.
On my last day, I finally saw an oto-ophthalmoscope. It was in the keeping of the head nurse, Clara, and available on request. Instead of relying on diagnostic equipment, or on the ultrasounds that could be ordered from a private office, the physicians relied heavily on physical exam skills.
Many male patients were admitted with large livers and bellies swollen by ascites (fluid in the abdominal cavity) due to cirrhosis or amoebic damage. My favorite physician-teacher frequently invited me to percuss these patients and discuss my findings. (I was given several remedial percussion lessons.) He was particularly anxious to have me see an advanced amoebal infection.
He said that in this area, with its high rates of diarrhea from Shigella, Giardia and E. Coli, people often ignore the symptoms of amoebas or are asymptomatic until they begin to cough up blood. This happens because amoebas, having colonized the liver, break through the diaphragm into the lung cavity.
Sadly, one of the most expensive, and therefore absent, commodities was paper goods. Mexico has to buy most of its paper. So there were no paper towels, or adult diapers, or paper gowns for patients. There were few paper booties or caps to use during surgery. For most chores there were cloth substitutes. Moreover, the paper toilet tissue in the bathrooms ran out after my first three days. In three weeks, it never reappeared.
I think that many women probably traveled with their own personal stock of paper, because tissue was in short supply all over town. Nevertheless, I began to see how infection control might be difficult.
This was brought home to me on a different afternoon when I was at the fancier hospital in town — one set up for gringos and Mexicans with insurance. This hospital was large and new but has the same constraints.
In their intensive care room, the nurses and I had to clean up the copious diarrhea of an American woman, a drug addict. She was being propped up in a leather armchair in an attempt to wean her from her ancient respirator. We used sheets and towels to mop up her liquid mess, and then called in an orderly, who mopped it up with the same stringy mop he used for the rest of the hospital’s floors.
I don’t remember if we used gloves, but I certainly remember that my first instinct to grab one of the two adult paper diapers from the shelf was the wrong one. In one moment, I had wiped out half of that day’s Depends.
Another paper good in short supply was books. The hospital had a small, locked library, and one of the internists sometimes brought his own books into the resident’s room, but there were no books near the ER or examining areas: no Physician’s Desk Reference, no Spanish equivalent of Harrison’s.
Sometimes, the lack of cash contributed to a lesser standard of care. The physicians were aware of this and saddened by it. Although all needles and sutures were of course disposable, not all tubing connections were; some American-made disposable parts had to be re-used, after autoclaving.
At the fancier hospital, across town, the internist there told me how distressed he was that he could not change catheters as often as he wanted; there simply weren’t enough sets available that month. One evening, in the emergency room, the nurse was told the lab could not do any more urine tests that night.
There was a lack of urine collection bottles, or strips, or some vital reagent. This kept them from doing a timely pregnancy test on Noemi, a young woman who had severe abdominal pain, an IUD, and sufficient shyness to give three different menstrual histories to each examining doctor in turn. As a result, the general surgeon took her in to exploratory surgery without knowing that she did in fact have an ectopic pregnancy.
On another day, I heard the radiologist hurriedly consulting with the medical director because he was out of all but the smallest size X-ray films.
In the year since I left Mexico, conditions have gotten worse. A retired physician in the community told me that the hospital has been unable to afford blankets for all the newborns. Allegedly, some have been sent home wrapped in newspapers.
Financial hardships for patients
The financial straits of the hospital were minor compared to the hardships of many of the patients. For the poorest residents of Mexico, there is no money for health insurance. All non-emergent care at the hospital must be pay-as-you-go, even though the rates were kept low.
Patients’ families have to make arrangements with moneylenders if they suddenly need to pay for medical care.
The physicians donate a lot of their time and loan their personal equipment, such as intensive care machinery. Still, it’s not enough help for all the patients.
One afternoon a woman brought in her five-year-old daughter because she had fractured her arm just above the elbow the day before. The orthopedist put the girl’s arm in a light cast to protect the arteries and nerves temporarily but explained that they would have to return in a few days with the money for the operation and the screws he would need for an internal fixation.
He said that he would bring in his own orthopedic surgical equipment, since the hospital only had tools for routine surgeries. As the mother and daughter left, he told me he was not at all certain they would return. Even though he had warned them that she could lose the use of the arm if they didn’t come, he said he had sent several other cases home that year and they had not returned. (He couldn’t say for sure that they had not taken their children to one of the larger hospitals two hours away in San Luis Potosi or Queretaro. But he was pretty sure that they had not.)
The $150 for the procedure and screws and hospital stay was probably out of their reach. One simple difference between Californian hospitals and the ones I observed in Mexico was that the billing day started at midnight rather than at noon.
Several times I saw patients who had been recuperating in the ER get discharged at midnight. One woman had come three hours by bus with her sick child, knew no one in town, and could not get a bus back until morning. They discharged her so that she could spend the night on the patio and not be charged an extra day.
Patients also lacked money to complete antibiotic treatment. The hospital staff were very worried about drug resistance. But the medicos pasantes could only provide a day or two of each drug, not a 10-day course; and they also suspected that if they gave 10 days, the family would use it until they felt better and then stop in order to have the drug available for the next person who got sick.
Another problem for rural patients was hygiene. There is so little water that nearly every rural patient came in covered with grime.
One day I escorted a woman into outpatient ophthalmologic surgery who had very dirty feet and legs. The surgeon calmly draped her upper body when she was on the table and created a sterile field for the surgery. But I could not help feeling a little odd about the proximity of the surgery and the dust.
Many patients had not been able to take real bath for months, so the nurses helped the most soiled people take a bath in a little room off to one side before they would let them be examined.
Everyone was very conscious of looking well-dressed. Noemi, who recovered well from her ectopic pregnancy, came in for a post-op checkup wearing a very fancy blue satin dress. But clearly she had been unable to wash it. It was shiny — and grimy.
Cultural differences
One of my goals in coming to the hospitals was to get a sense of what Mexican citizens who might come to the U.S. expected from their medical providers, based on care they had received in Mexico.
Knowing that Mexican women can be quite modest, my first surprise was that the ER lacked curtains around its beds, and ER patients were not often provided with gowns or drapes during exams. It was difficult for many of the women, since both the ER examining room and the holding bedroom had room for three patients, who were not segregated sexually.
The women would hold up whatever they could to shield their bodies from the other patients and physicians. Some patients also have little experience with hospitals, hospital procedures, or donating blood.
One day, I came in to find a teenage girl in one of the ER holding beds, in agony from a black widow spider bite she had gotten the day before. Her joints were so painful that she could not stand up, and therefore could not go to the toilet.
There was no curtain around her bed, but finally, after several hours, it became so clear that she had to urinate that I got a bedpan from the ER staff, who were occupied with other patients.
I tried to explain to her how to use it (this was definitely a language challenge), but she just didn’t believe that she wouldn’t get herself wet, and since she had no sheet on her bed, she was reluctant anyway.
She was too modest to try it for almost another hour and then she tried to crouch over it. It was painful to see her trying to put weight on her feet, but we could not convince her that it would work.
The doctors told me they also have a hard time getting people to donate blood. The nearest blood bank was an hour and a half away and oversubscribed, so patients must have family members and friends donate for them.
According to the doctors, many rural people don’t believe that their blood has regenerated after they give it. Therefore, although many people will donate once for a loved one, they are afraid to do it again.
The tragedy of errors
On my last day in the hospital, I was shown a very weak young woman walking in the hall. My instructor told me that some poorly trained general doctor had apparently prescribed the wrong amount and inappropriately long course of chloramphenicol for her, and now she had aplastic anemia. Her hemoglobin had risen from 2 to 4, after transfusion. But she was out of donors, and out of time. She would almost certainly not recover.
My preceptor was particularly candid about this case because he wanted me to understand how necessary it was for me and my fellow trainees to find ways to stay informed about changes in the standard of practice.
Most physicians in Mexico have been made aware of the risks of using chloramphenicol, a common antibiotic. This woman’s general physician presumably was not.
My preceptor works diligently to train his residents and pasantes to treat accurately and safely on their own. He knows they may easily end up practicing without the safety of libraries, current journals, or access to second opinions.
Into the future
My visits to San Miguel provided a brief, unique, informative window into Mexico’s public health sector. Now I hear that this already strained system is undergoing still more transition.
Recently, National Public Radio discussed the Mexican government’s plans to privatize its public health hospitals. Some say that the financial strain of supporting the 80% of Mexicans who are uninsured is now more than the government can bear. It is unclear if the new approach will improve or worsen medicine for the poor.
My four weeks of informal observation gave me tremendous respect for the courage of the hard-working public health doctors I met. I wish them well in their ongoing struggle to treat, and teach, increasingly adverse conditions. I very much appreciated the chance to observe their efforts and achievements.