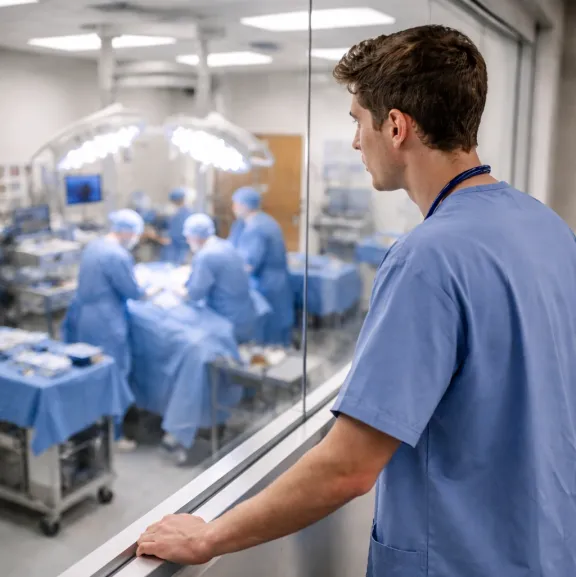
From Ideal Scenarios to Operating Room Chaos
Entering clinical environments for the first time as a medical student, I expected to hear common phrases of wisdom. I certainly heard my fair share, with classics such as “When you hear hooves, think horses instead of zebras,” superstitions such as “Never say the Q-word [quiet],” and self-care idioms such as “eat when you can.”
But the one that I heard the most was not one that shows up in lists of common wisdom. I heard it in several settings from family medicine clinic to a thoracic surgery operating room, from different levels of the healthcare hierarchy including attending physicians, nurses, technicians, and resident physicians. With striking consistency, in the first three years of my medical training, I frequently hear “It’s not usually like this.”
The first time I heard this phrase was during a wedge resection of a lung lobe in thoracic surgery. Our patient had a lung nodule seen on a screening CT scan and was recommended the procedure due to her risk of cancer.
The approach to the surgery was to first inject Indocyanine Green (ICG) dye using a bronchoscope to help visualize the nodule, and then laparoscopically resect the portion of the lung. The bronchoscopy was delayed due to equipment malfunctions, and when it came time to visualize the nodule, the surgeons could not find the nodule of interest.
Over the course of the surgery, they had to open another incision for the attending surgeon even to use his finger to locate the nodule. It was at that point that the circulating nurse told me, “It’s not usually like this; usually these surgeries are smoother.” The nodule was successfully removed and found to be early-stage cancer, but only after finishing two hours behind schedule.
The first time I heard that phrase, I didn’t think much of it. But the same wording for the same idea kept coming up throughout my clinical experiences. I heard it from my psychiatry preceptor when our morning clinic had four no-shows, and I did not see any patients in the half day I was present.
I heard it from a nurse when an upper endoscopy I observed was terminated when the patient’s gag reflex could not tolerate the endoscope despite maxing her dose of sedatives. I heard it in a family medicine clinic when multiple patients broke down in tears during my visits with them. The car driver of the lung transplant service told me this when our car was caught in Bay Bridge traffic with a pair of lungs in a cooler in the trunk.
Have my teams felt the need to shield me from the inconvenient realities of healthcare? Or perhaps their motives are less cagey: maybe it’s selective memory as a coping mechanism.
Either way, we would do better to prepare medical students for the reality of the myriad hiccups we will inevitably encounter. During the preclinical years of medical school, students are taught medicine in ideal scenarios. Insurance challenges never play a role in the treatment of our fictional patients. Our surgical scenarios never discuss logistical delays in care.
We occasionally discuss social determinants of health in the development of disease but never dissect how to address those within the constraints of a health system strapped by limited resources. We sometimes discuss bias in medicine but never discuss what people mean when they say a patient is “difficult.”
I imagine my team members were looking out for me when they insisted that their days are usually smoother. However, we do a disservice to trainees by trying to shield them from the realities of healthcare.
Studies suggest that empathy is highest among medical students at the beginning of their training. The earlier that students can be exposed to the rocky realities of healthcare and be engaged in discussions about how to approach these issues from a place of empathy and stability, the better we can be prepared for adverse events when they occur.